Types of Mesothelioma
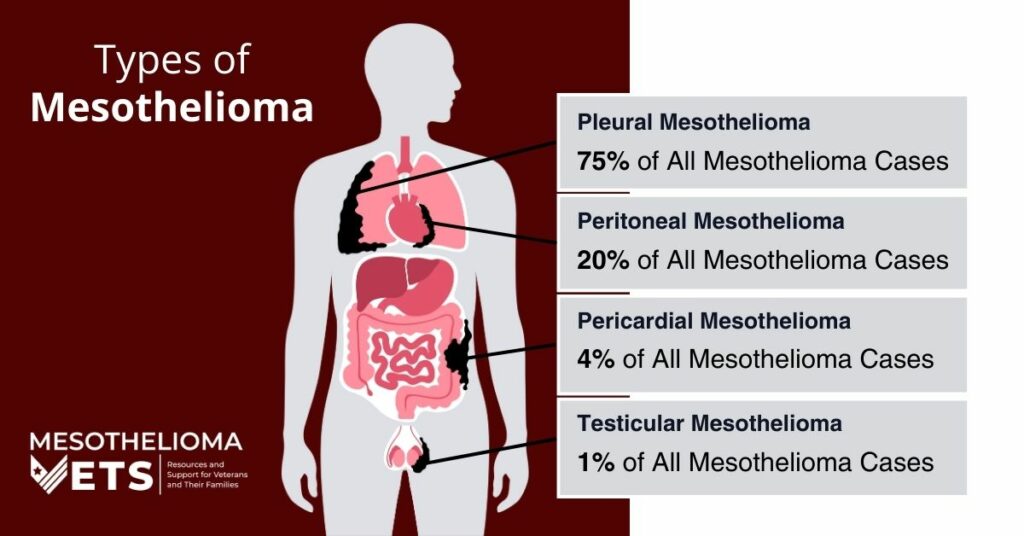
Mesothelioma is a rare cancer affecting the mesothelium, or the thin layer of tissue that surrounds the lungs, abdomen, and heart. The disease is classified into three types, depending on where the tumors are located in the body. Patients are diagnosed with pleural, peritoneal, or pericardial mesothelioma.

What Are the Three Types of Mesothelioma?
There are three main types of mesothelioma. These types are pleural mesothelioma, which affects the lining of the lungs; peritoneal mesothelioma, which affects the lining of the stomach; and pericardial mesothelioma, which affects the lining of the heart. The location of the tumors determines the kind of mesothelioma a patient has.
Doctors also diagnose mesothelioma based on the types of cells found within the tumor. Location and cell types are both factors in a patient’s treatment plan and overall prognosis.
Pleural Mesothelioma
This type affects the chest cavity and lining of the lungs and is the most common form of the disease. Between 70 and 90 percent of patients receive this diagnosis. The disease develops as a result of exposure to asbestos through inhalation. Microscopic fibers within asbestos dust cling to the pleura, the lining of the lungs. Eventually, these toxic fibers start to irritate the pleura, causing inflammation and creating scar tissue. Decades later, those cells can mutate and form malignant tumors.
The average life expectancy for veterans with this form is between 8 and 21 months. However, those numbers can vary depending on cell type and stage or how far tumors have spread.
Pleural Mesothelioma: Symptoms
- Chest pain
- Fatigue
- Fever
- Persistent dry cough
- Shortness of breath
- Weight loss
Most patients experience pleural effusion, or a buildup of fluid around the lungs, which can make it tough to breathe.
Mesothelioma symptoms often mirror other common illnesses, including the flu, pneumonia, and other cancers. For this reason, it’s hard to detect. Doctors must rely on a combination of imaging tests, blood tests, and biopsies to ensure a correct diagnosis.
Needle biopsies, like pleural biopsies or thoracentesis, allow doctors to collect samples for testing. They are often used to remove excess lung fluid to help relieve breathing discomfort. Other common tests include camera-assisted biopsies, like thoracoscopies or mediastinoscopies, or a type of surgical biopsy called a thoracotomy, where doctors will take an actual sample of the tissue for further study. A tissue biopsy is the best way to make a definitive diagnosis of pleural mesothelioma.
Pleural Mesothelioma: Treatment
A patient’s treatment plan may vary depending on how far the disease has spread but will usually include a multimodal treatment plan or combination of therapies, including:
The two primary surgeries for pleural mesothelioma are pleurectomy decortication, which involves removing the lining of the chest and lungs, in addition to any visible tumors, and extrapleural pneumonectomy, where doctors remove the entire lung, the lining of the chest and heart, as well as portions of the diaphragm. Other procedures, like pleurodesis and thoracentesis, are used to remove excess lung fluid to make breathing easier.
Patients may undergo chemotherapy treatments before or after surgery to reduce or destroy cancer cells. The most common chemotherapy combination is ALIMTA® and cisplatin. Depending on the patient, physicians may use chemotherapy instead of surgery. Chemotherapy may be used as an aggressive, potentially curative treatment or as a palliative treatment to improve the quality of life for late-stage patients.
Radiation is also a standard therapy used before, during, or after surgery to control and reduce the spread of tumors. It’s also one of the many types of treatment used to mitigate symptoms in pleural mesothelioma patients who are not candidates for surgery.
Immunotherapy is a relatively new treatment option that utilizes the body’s immune system to attack cancer cells. Some patients may benefit from certain immunotherapy drugs or therapies.
Veterans who were diagnosed with mesothelioma may be eligible for VA compensation. To find out if you qualify, speak with a patient advocate today.

Peritoneal Mesothelioma
This type affects the lining of a patient’s abdomen or peritoneum. Between 10 to 30 percent of patients receive this diagnosis, making peritoneal the second most common form. It’s also caused by asbestos exposure, but when the fibers are somehow ingested. Doctors believe patients either swallow the dust directly or inhale it and then swallow the microscopic fibers. Once inside the body, asbestos fibers become lodged in the peritoneum or stomach lining, causing scar tissue and inflammation that leads to cancerous tumors in the abdominal cavity.
This type has a better prognosis as compared to others. Survival rates depend on the stage and cell type, but the average life expectancy for patients with malignant peritoneal mesothelioma is between 34 and 92 months.
Peritoneal Mesothelioma: Symptoms
- Abdominal distension
- Abdominal pain
- Diarrhea
- Fatigue
- Fever
- Hernia
- Nausea or vomiting
- Weight loss
Most patients also experience ascites, or a buildup of fluid in the abdomen, which can cause additional pain and bloat.
Symptoms can mirror those of other abdominal illnesses — such as IBS — as well as stomach or ovarian cancer. This can make the disease difficult and time-consuming to diagnose. As with pleural mesothelioma, doctors will use imaging tests, blood tests, and biopsies. Patients may require a specific needle biopsy, called paracentesis, to remove and test abdominal fluid or a camera-assisted biopsy, such as a laparoscopy or peritoneoscopy. In some patients, a surgical biopsy, called a laparotomy, may be necessary if other, less-invasive biopsies fail to provide a definitive diagnosis.
Peritoneal Mesothelioma: Treatment
Doctors recommend a multimodal treatment approach for peritoneal mesothelioma, depending on how far the disease has progressed. It can include chemotherapy, radiation, surgery, and, in some cases, immunotherapy or a combination.
The most common surgery for malignant peritoneal mesothelioma is a combination of cytoreductive surgery to remove all of the visible tumors in the abdominal cavity and Hyperthermic Intraperitoneal Chemotherapy (HIPEC), a heated chemotherapy wash placed inside the abdomen to kill any remaining cancer cells. Radiation is often used before or after to shrink or reduce tumors and prevent cancer recurrence.
As with pleural mesothelioma, chemotherapy and radiation are also used as palliative treatment options to mitigate symptoms in late-stage patients who aren’t candidates for cytoreductive surgery and HIPEC. Paracentesis is often used to remove fluid that has built up in the abdomen to reduce abdominal pain and swelling.
Veterans with mesothelioma can take action without affecting their benefits.

Pericardial Mesothelioma
This type develops inside the lining of the heart or the pericardium. It affects less than 5 percent of patients, making it the rarest type. Doctors often can’t pinpoint the exact cause but believe asbestos fibers are either ingested or inhaled, then reach the heart through the blood or lymphatic system. There, they become embedded in the heart lining, creating scar tissue and tumors on the lining of the heart sac.
The majority of pericardial mesothelioma cases go undiagnosed; it’s usually only discovered during surgery or after death. The prognosis is poor, and the average life expectancy is under one year.
Pericardial Mesothelioma: Symptoms
- Arrhythmia
- Chest pain
- Fatigue
- Heart murmur
- Weight loss
Patients may also experience pericardial effusion, a buildup of fluid around the heart, which can lead to chest pain and breathing difficulties.
Other cardiac illnesses, like heart disease and inflammation of the heart muscles, have similar symptoms to pericardial mesothelioma. This can make it difficult to diagnose. Similar to pleural and peritoneal mesothelioma, the diagnostic process includes imaging scans, blood tests, and fluid and tissue biopsies. Doctors who suspect pericardial mesothelioma may order an echocardiogram, a test that relies on sound waves to assess heart function, or a type of needle biopsy called pericardiocentesis.
Pericardial Mesothelioma: Treatment
Treatment for pericardial mesothelioma depends on the patient’s health and how far the cancer has progressed. Curative options include a pericardiectomy, a surgery that removes part or all of the pericardium, or chemotherapy with cisplatin. Palliative care treatments for those who can’t have surgery include pericardiocentesis, also referred to as a pericardial tap, and percutaneous balloon pericardiotomy. Both of these procedures relieve pericardial effusion, or excess fluid, around the heart sac. Chemotherapy is also used to slow the growth of tumors in late-stage patients to alleviate specific symptoms, like chest pain or difficulty breathing.